Tag: Dysphagia Rehabilitation
-

Strength vs. Skill in Swallowing: Rethinking Dysphagia Therapy Approaches
Should dysphagia therapy focus on skill training or strength training? Learn how both approaches impact swallowing rehabilitation, why exercise science principles matter, and what research says about effective therapy strategies for SLPs.
Written by
·
-

MD Anderson Bootcamp for Swallowing
Dysphagia post-head and neck cancer treatment is a significant challenge for clinicians. MD Anderson’s 2012 Dysphagia Boot Camp offers a reactive therapy for patients with severe swallowing difficulties. Through intensive, multidisciplinary approaches, participants engage in personalized rehabilitation aiming to improve safety, efficiency, and quality of life, resulting in notable improvements in swallowing outcomes.
Written by
·
-

Nutrition Essentials for Modified Diets
Nutrition is vital for health, especially for individuals on modified diets, who are at risk of malnutrition. Macronutrients (carbohydrates, proteins, fats) and micronutrients (vitamins, minerals) play crucial roles. Strategies such as food fortification, small frequent meals, and hydration can enhance nutritional intake, ensuring patients maintain health and well-being despite dietary restrictions.
Written by
·
-

Intensive Dysphagia Rehabilitation (IDR)
Intensive Dysphagia Rehabilitation (IDR) streamlines therapy for patients with moderate to severe dysphagia through evidence-based protocols leveraging neuroplasticity. By focusing on targeted swallowing exercises and patient adherence, IDR enhances treatment efficacy, improving patient outcomes and compliance. It marks a significant shift from compensation to active rehabilitation in dysphagia therapy.
Written by
·
-
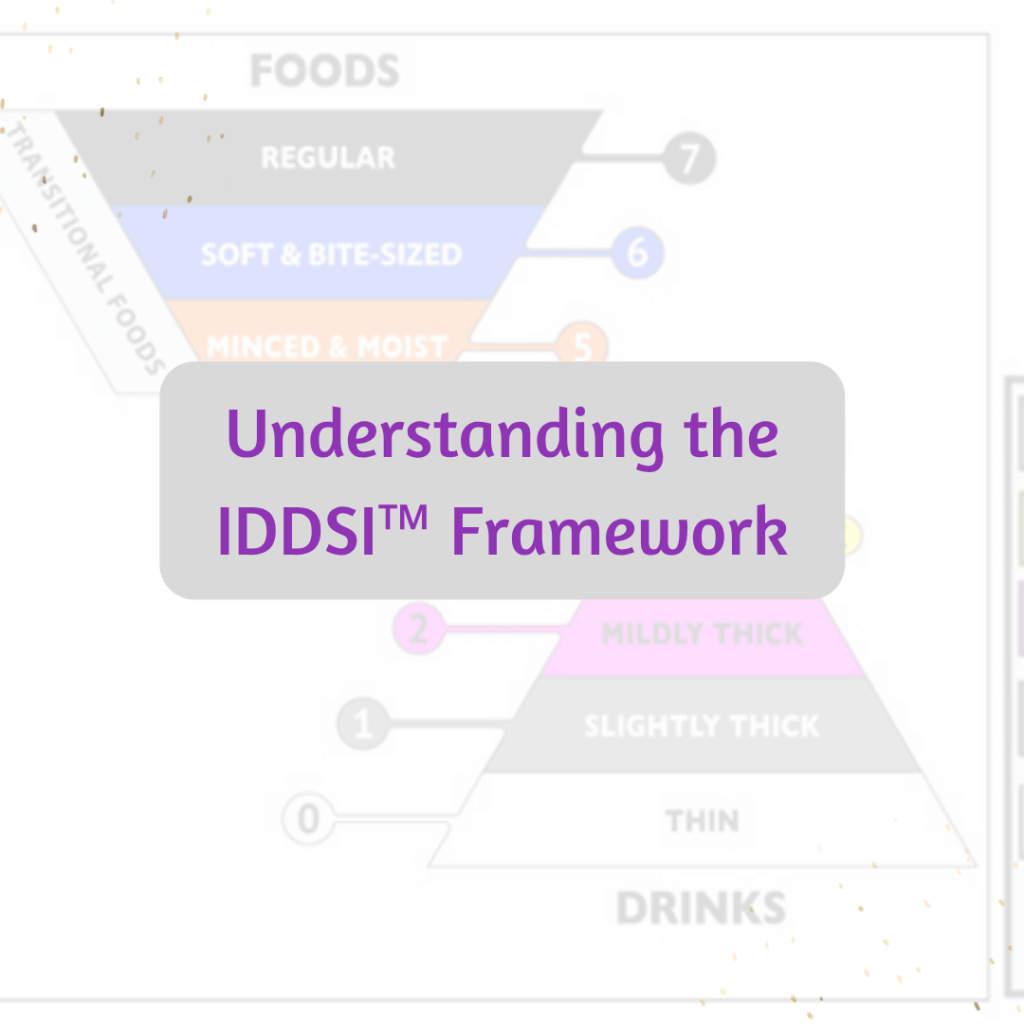
Understanding the IDDSI™ Framework
The International Dysphagia Diet Standardisation Initiative (IDDSI™) provides a unified system for food and drink consistencies, enhancing patient safety. It replaces the National Dysphagia Diet, offering clear levels for drinks and foods, minimizing risks. Resources such as testing cards and guides support implementation and training in diverse healthcare settings.
Written by
·
-

Not Nectar (Mildly) Thick: The Truth About Carbonated Beverages and Dysphagia
Carbonated beverages are being explored in dysphagia management as a sensory strategy to enhance swallowing safety, not as thickened liquids. Research indicates carbonation may stimulate the Trigeminal nerve, potentially improving swallow function for some patients. However, effectiveness varies individually, necessitating personalized assessment rather than substitution for thickened liquids.
Written by
·
-

Compliance or Choice? Rethinking the “Noncompliant” Dysphagia Patient
The post discusses evolving perspectives on patient noncompliance in dysphagia management. It suggests reframing noncompliance as patient choice, emphasizing the importance of education and support rather than discharge. Highlighting that not all aspirators contract pneumonia, it advocates for individualized approaches in therapy that empower patients to make informed decisions about their care and safety.
Written by
·