Author: Tiffani Wallace-SLP and Certified Nutrition Coach
-

30 Facts About Dysphagia to Raise Awareness and Improve Patient Care
June is Dysphagia Awareness Month, highlighting the condition affecting millions. Dysphagia, or difficulty swallowing, can stem from various underlying issues and leads to serious health risks. Speech-Language Pathologists play a vital role in diagnosis and treatment. Raising awareness about dysphagia improves outcomes for patients, caregivers, and healthcare providers alike.
Written by
·
-

Nutrition Essentials for Modified Diets
Nutrition is vital for health, especially for individuals on modified diets, who are at risk of malnutrition. Macronutrients (carbohydrates, proteins, fats) and micronutrients (vitamins, minerals) play crucial roles. Strategies such as food fortification, small frequent meals, and hydration can enhance nutritional intake, ensuring patients maintain health and well-being despite dietary restrictions.
Written by
·
-

Modern Dysphagia Cooking: Turn Family Favorites into Dysphagia-Friendly Dishes
Simply Thick has released a cookbook featuring dysphagia-friendly recipes compliant with IDDSI levels 4, 5, and 6. It includes simple pureeing techniques for common foods, alongside informative chapters on dysphagia and nutrition. This resource aids families, patients, and caregivers in preparing compliant meals, enhancing dietary understanding and meal preparation.
Written by
·
-

SWIK Oral Suction System
The SWIK Oral Suction System is an innovative solution for managing oral secretions. Unlike traditional suction methods, it uses a small sponge to collect secretions hands-free. Its design emphasizes user comfort and dignity. Created by hairdresser Rebecca Altounian, it offers a discreet alternative for those needing assistance.
Written by
·
-

Intensive Dysphagia Rehabilitation (IDR)
Intensive Dysphagia Rehabilitation (IDR) streamlines therapy for patients with moderate to severe dysphagia through evidence-based protocols leveraging neuroplasticity. By focusing on targeted swallowing exercises and patient adherence, IDR enhances treatment efficacy, improving patient outcomes and compliance. It marks a significant shift from compensation to active rehabilitation in dysphagia therapy.
Written by
·
-

Head and Neck Cancer and Dysphagia: Treatment Options and Timing
Effective management of dysphagia in head and neck cancer patients involves early assessment and initiation of swallowing therapy alongside treatment. Various strategies, including rigorous swallowing exercises and innovative programs like MD Anderson’s Swallowing Boot Camp, show promise in improving swallowing function and quality of life, despite challenges in standardization and adherence.
Written by
·
-

Math and Dysphagia
The blog post by George Barnes and Doreen Benson emphasizes the importance of incorporating statistics into speech-language pathology (SLP) practices, specifically for treating dysphagia. It discusses common cognitive biases affecting clinical decision-making and stresses the need for a more analytical approach in evaluating patient risks and benefits, promoting better outcomes in care.
Written by
·
-
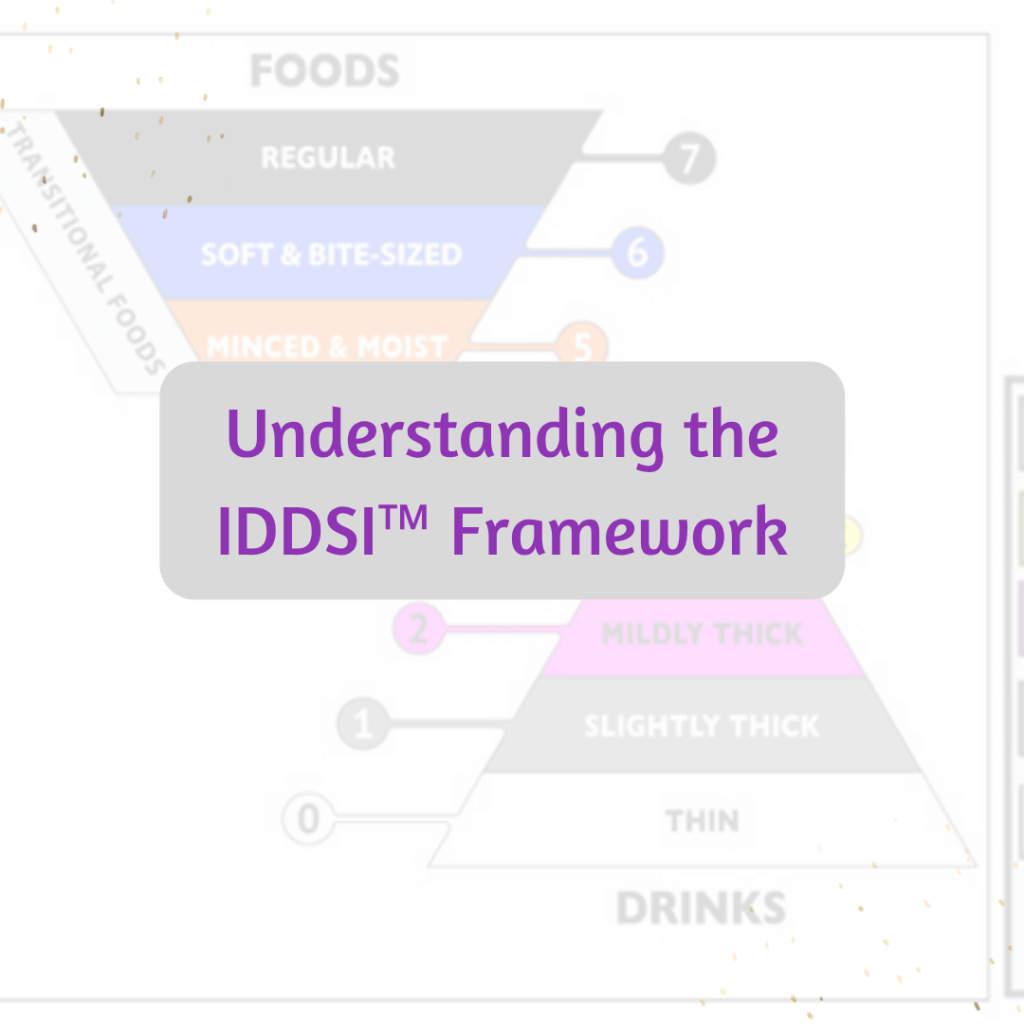
Understanding the IDDSI™ Framework
The International Dysphagia Diet Standardisation Initiative (IDDSI™) provides a unified system for food and drink consistencies, enhancing patient safety. It replaces the National Dysphagia Diet, offering clear levels for drinks and foods, minimizing risks. Resources such as testing cards and guides support implementation and training in diverse healthcare settings.
Written by
·
-

Measuring Outcomes for Success…..What are You Using?
The Dysphagia Toolbox offers valuable tools for dysphagia assessment and treatment. Various free outcome measures like questionnaires and screening tools support clinicians in evaluating patients effectively. These assessments track progress and ensure reliable evaluations, which are essential for optimal dysphagia management and documentation in compliance with healthcare standards.
Written by
·
-

How Cognition Influences Swallowing Safety
Cognition significantly influences swallowing abilities, with cognitive decline leading to increased risks of aspiration and malnutrition. A clinical case illustrated that normalizing sodium levels improved swallowing function. Studies show that cognitive assessments predict aspiration risks, highlighting the importance of screening patients’ orientation and command-following before dysphagia evaluations to ensure safety in oral intake.
Written by
·