Category: Thickened Liquids
-

The Free Water Protocol: Why Sometimes All a Patient Wants Is Just… Water
The Free Water Protocol allows certain patients, particularly those on thickened liquids or NPO status, to safely consume regular water between meals. Emphasizing hydration and patient dignity, it incorporates oral care and eligibility criteria. Research shows it enhances hydration and patient satisfaction, countering dehydration and fostering a sense of normalcy in care.
Written by
·
-
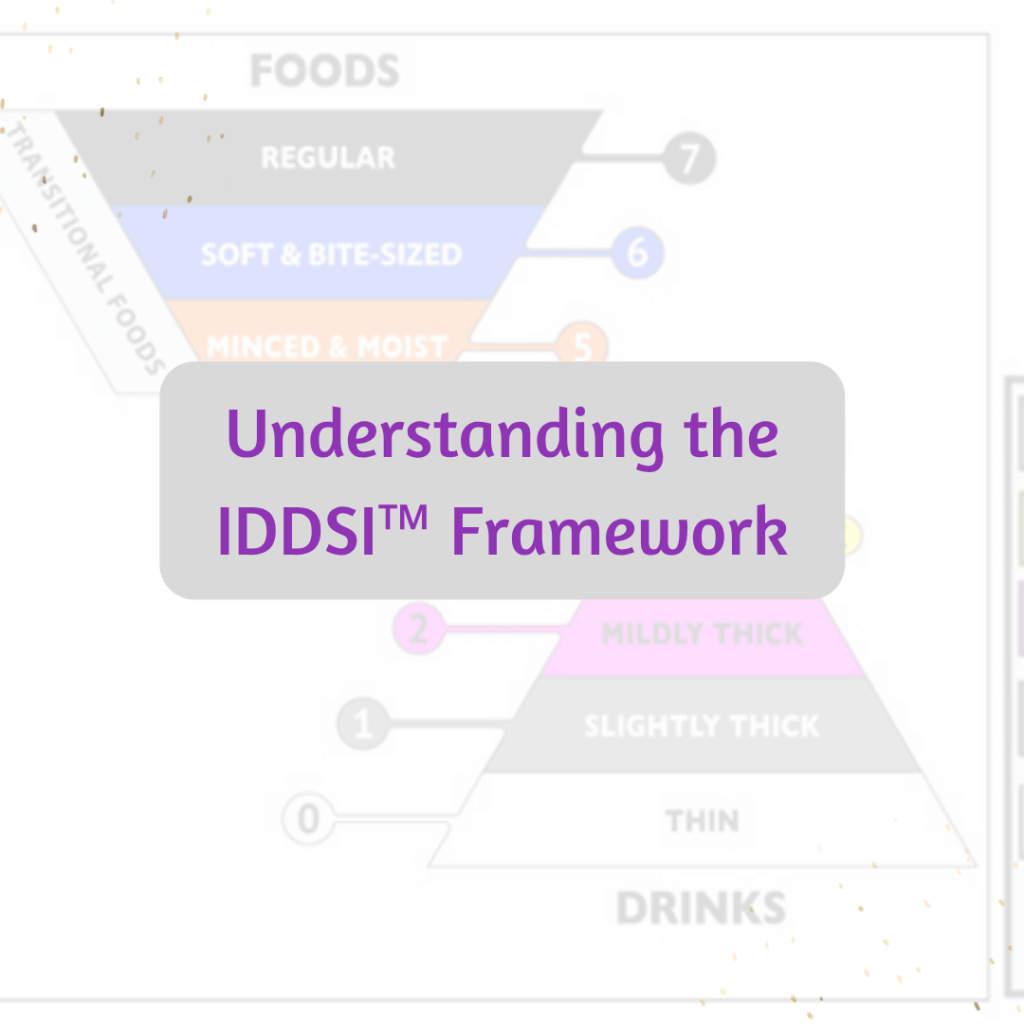
Understanding the IDDSI™ Framework
The International Dysphagia Diet Standardisation Initiative (IDDSI™) provides a unified system for food and drink consistencies, enhancing patient safety. It replaces the National Dysphagia Diet, offering clear levels for drinks and foods, minimizing risks. Resources such as testing cards and guides support implementation and training in diverse healthcare settings.
Written by
·
-

The Cost of Thickened Liquids
Thickened liquids are commonly used in dysphagia management, but there’s a growing interest in alternatives that may offer safer options. While they can be effective, costs of thickening agents are significant and patient preferences vary. The focus should be on individualizing care to balance hydration, health, and quality of life for patients.
Written by
·
-

Trying Gelmix: A USDA Organic Thickener for Dysphagia
Gelmix is a USDA Organic thickener designed for infants and children under three, suitable for thickening liquids like breast milk and formula. Composed of organic carob bean gum, tapioca maltodextrin, and calcium carbonate, it’s effective when mixed in warm liquids. Contraindicated for premature infants and those with galactomannan allergies, it offers gradual thickening and a…
Written by
·
-

Thickened Jello
The article discusses the introduction of thickened Jello, developed with SimplyThick, as a solution for patients with dysphagia who crave traditional Jello. The author shares their experience testing the product, noting its pleasant taste and ability to maintain consistency. Instructions for making thickened Jello at home are also provided.
Written by
·
-

The Great Thickener Challenge
The Great Thickener Challenge explores various thickening options for patients needing modified liquids. After sampling several brands, participants preferred Simply Thick due to its pleasant taste and consistency. Concerns about the use of thickened liquids impact hydration and aspiration risks, emphasizing the need for careful recommendations and education on dysphagia.
Written by
·